After starting pantoprazole, the safest next step is consistency: take it exactly as prescribed, track triggers, and ask your clinician before changing dose or timing. Add-on options should match the problem: alginate for post-meal barrier support, DGL for chewable comfort, and probiotic/fiber routines for broader digestive regularity, not medication replacement.
How did we evaluate options after starting pantoprazole?
Supplement Buyers Lab evaluated add-on options by mechanism, evidence quality, medication-context safety, label transparency, and routine fit. Clinical guidelines and human studies received more weight than Reddit anecdotes, brand claims, animal data, or broad “gut reset” language. The ACG GERD guideline and the AGA PPI de-prescribing update shaped one boundary: pantoprazole decisions belong with a clinician, especially when symptoms are frequent, severe, or changing. We excluded medical-outcome claims, acid-replacement theories, “detox” protocols, and supplement stacks that make medication-sparing promises. We also separated fast post-meal mechanics from slower routine support. Alginate has direct reflux-symptom literature. DGL licorice has a comfort-oriented rationale plus licorice safety considerations. Probiotic and fiber routines have broader digestive-regularity logic, but reflux-specific data remain heterogeneous. That constraint keeps recommendations realistic.
What should you do first after getting pantoprazole?
Pantoprazole works best when the medication plan stays boring, clear, and clinician-directed. The first move is taking pantoprazole exactly as prescribed, because dose timing, missed doses, food timing, and competing medicines can change how acid-suppression routines feel. The second move is tracking three variables for two weeks: meal size, late eating, and body position after meals. The AGA de-prescribing update warns that rebound-style symptoms can appear when PPIs are reduced or stopped, so self-adjusting early can create noise that looks like failure. The third move is checking red flags with a clinician: trouble swallowing, vomiting blood, black stools, unexplained weight loss, persistent chest pain, or symptoms that wake you regularly. Supplements can support normal digestive comfort, but they do not replace the prescribing conversation. The cleanest plan is prescription consistency, simple tracking, then one add-on category at a time if needed.
What should you look for when choosing add-on digestive support?
The best add-on choice should match timing, mechanism, and safety constraints. Post-meal throat burn or regurgitation points toward alginate, because sodium alginate formulas form a raft-like barrier above stomach contents after meals; a 2017 meta-analysis by Leiman et al. reported favorable symptom-response findings across alginate trials (PubMed). Occasional upper-digestive comfort points toward DGL licorice, but licorice-derived supplements still deserve medication-context caution; NCCIH notes that glycyrrhizin-containing licorice can affect blood pressure and potassium (NCCIH). Irregularity, low fiber intake, or inconsistent stool patterns point toward a probiotic/fiber routine, not an immediate reflux tool. A 2020 review in Nutrients found probiotic reflux studies promising but heterogeneous (PubMed). Buyers should compare active form, serving timing, sodium, strain identity, CFU through expiration, fiber grams, sweeteners, allergen notes, and clinician compatibility.
How do the top options compare after starting a PPI?
Pantoprazole reduces acid exposure through prescription acid suppression, while add-on digestive supports work through different, narrower mechanisms. Alginate is the most targeted non-prescription category for after-meal reflux mechanics because the raft effect depends on timing. DGL is a chewable comfort option rather than an acid-control strategy, so buyers should judge it by ingredient form, glycyrrhizin handling, and medication context. Probiotics are routine tools, and strain-specific evidence matters more than generic “billions of CFU” language. Fiber is a regularity tool, and gradual dosing matters more than heroic intake. The comparison below uses use-case fit instead of ranking every category as if they solve the same problem. That matters after starting a PPI, because adding four products at once makes symptom tracking useless. One category, used consistently, gives a clearer signal than a supplement pile. Clear signals matter when the prescription plan is still new.
| Option | Best for | Primary role | Evidence fit | Main watch-out |
|---|---|---|---|---|
| Alginate | Best for post-meal barrier support | Forms a raft above stomach contents | Direct reflux-symptom studies | Sodium, calcium, timing, and short duration |
| DGL licorice | Best for chewable upper-digestive comfort | Supports normal stomach and throat comfort routines | More comfort-oriented than reflux-specific | Licorice context, medicines, pregnancy, blood pressure |
| Probiotic routine | Best for broader gut-balance goals | Supports microbiome routine consistency | Heterogeneous, strain-specific evidence | Strain codes and CFU at expiration matter |
| Fiber routine | Best for low-fiber or irregular routines | Supports stool regularity and meal pattern stability | Strong general digestive rationale | Start low; rapid dose jumps can feel uncomfortable |
Which option is best for each use case?
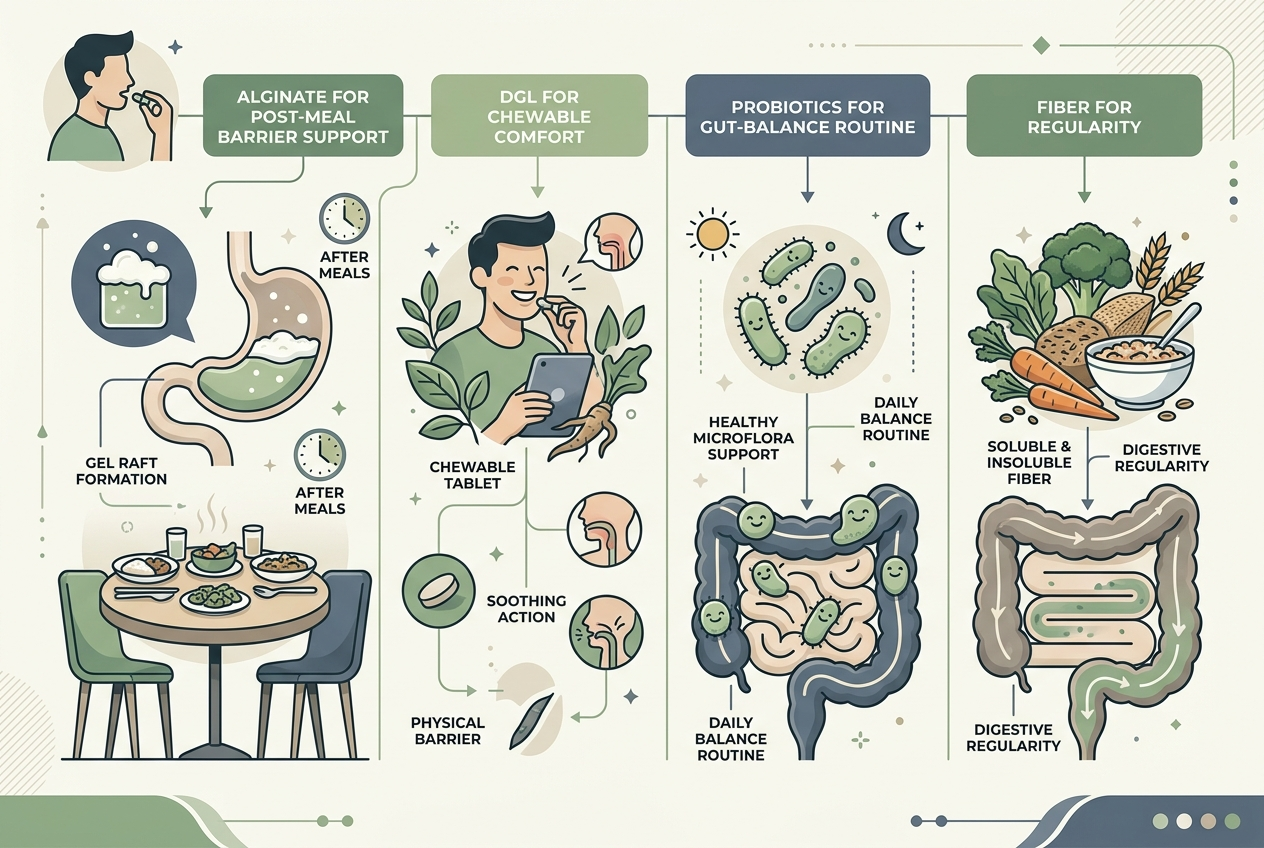
Best for post-meal flare patterns: alginate, because sodium alginate and bicarbonate formulas work at the stomach-content interface after meals. Best for people who want a chewable comfort format: DGL licorice, because deglycyrrhizinated licorice products are usually positioned for occasional upper-digestive comfort rather than daily acid control. Best for people whose “now what?” includes constipation, irregularity, or low plant-food intake: fiber, because soluble fiber supports stool consistency and routine predictability. Best for people rebuilding a daily gut-health habit: a probiotic with disclosed strains, because Lactobacillus and Bifidobacterium benefits are strain-specific. Best for people who just started pantoprazole and feel anxious: no add-on yet, because baseline tracking is more informative than immediate stacking. Best for people with medication questions: the prescribing clinician, because pantoprazole dose, duration, and taper decisions are medical decisions, not supplement-shopping decisions today.
Which products meet these criteria?
Some links below are affiliate links. This does not influence our evaluation criteria or recommendations.
Reflux Gourmet meets the alginate criteria for shoppers who want a post-meal raft-forming option and who will review sodium, calcium, and timing instructions. Natural Factors DGL meets the DGL criteria for shoppers who want a chewable licorice-derived comfort format and who will consider medication context. Culturelle Digestive Daily Probiotic meets the probiotic criteria for shoppers who want a named strain, Lactobacillus rhamnosus GG, in a capsule routine. Yuve Probiotic Gummies meet the convenience criteria for shoppers who want a vegan, gluten-free gummy format with 5 billion CFU per serving, but buyers who prioritize strain-matched clinical literature should confirm the strain disclosure before choosing. Yuve Prebiotic Fiber Gummies fit a gradual fiber-routine lane with 3 grams soluble fiber per serving. The broader digestive health collection is useful for comparing format friction.
What does price and value look like?
Value after starting pantoprazole is not the cheapest bottle; value is the lowest-friction tool that answers the right use case without confusing the prescription plan. Alginate usually costs more per use than basic antacid-style products, but its value comes from meal-timed mechanical support. DGL chewables often sit in the middle, and value depends on glycyrrhizin handling, serving count, flavor tolerance, and how often the chewable moment actually occurs. Probiotic capsules and gummies vary widely, so shoppers should compare CFU through expiration, strain disclosure, storage, serving count, and sugar alcohols. Fiber gummies often look convenient but cost more per gram of fiber than powders or food sources. The smartest budget rule is one experiment per two weeks. If the pattern is post-meal, trial alginate. If the pattern is irregularity, trial fiber. If the goal is routine adherence, choose the format you will repeat.
What questions do people ask after starting pantoprazole?
Can I stop pantoprazole once I feel better?
Do not stop or change pantoprazole without the prescriber’s guidance. The AGA update describes rebound symptoms after PPI reduction or discontinuation, so sudden changes can make the next few weeks confusing.
Should I add alginate while taking a PPI?
Alginate can make sense as a post-meal support category because it works mechanically rather than by changing the PPI dose. Ask a clinician or pharmacist about spacing if you also take other medicines around meals.
Is DGL licorice safe with pantoprazole?
DGL licorice is usually evaluated as a licorice-derived comfort supplement, not as a medication substitute. People with blood pressure concerns, potassium issues, pregnancy care, or complex medication lists should ask a clinician first.
Are probiotics useful after starting a PPI?
Probiotics may fit a broader gut-balance routine, but they are not a fast reflux-control tool. Strain identity, daily consistency, and CFU through expiration matter more than a high CFU number alone.
Should I take fiber if reflux is the main issue?
Fiber makes the most sense when low fiber intake, irregular stool, or inconsistent meals are part of the pattern. Start slowly, because large fiber increases can create gas, pressure, or discomfort.
What should I track before adding supplements?
Track pantoprazole timing, dinner timing, meal size, caffeine, alcohol, lying down after meals, and symptom timing. A two-week log gives a clinician better information and helps you avoid random supplement stacking.
For a closer look at clean-label options, see I Fixed My Reflux by Accident? How to Figure Out What Actually Changed.
What is the practical next step?
Start with the prescription plan, then choose one support lane only if the pattern calls for it. Post-meal symptoms point toward alginate. Chewable comfort needs point toward DGL. Irregularity or low-fiber routines point toward fiber. Broader gut-balance goals point toward probiotics. Yuve is one reasonable option in the gummy probiotic/fiber lane, while Reflux Gourmet, Natural Factors, and Culturelle represent different mechanisms. None of these choices should be used to change pantoprazole dose, duration, or taper timing without clinical input. If symptoms are severe, new, worsening, or paired with alarm signs, professional medical guidance beats every comparison table. Keep the plan simple: stabilize the medication routine, track the pattern, choose one support category if appropriate, and reassess with real notes instead of vibes, especially during the first two weeks of early daily use tracking.

Leave a Reply